The prostate – ????? ?????? (from Ancient Greek ?????????, prostát?s, literally “one who stands before”, “protector”, “guardian”) is a compound tubuloalveolar exocrine gland of the male reproductive system in most mammals. It differs considerably among species anatomically, chemically, and physiologically. So, know in detail about the prostate, structure, divisions, development, functions, and clinical significance. Siddha Spirituality of Swami Hardas Life System has a pious intention of creating awareness about prostate among our valuable readers. In case, any problem faced about, we also recommend undergoing training of Swami Hardas Life System.
Prostate Structure (????? ?????? ?? ??????)
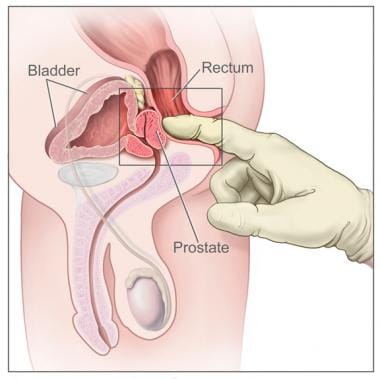
The classical description of a healthy human male prostate portrays it as slightly larger than a walnut. The mean weight of the normal prostate in adult males is about 11 grams, usually ranging between 7 and 16 grams. A study stated that volume among patients with negative biopsy is related significantly with weight and height, so it is necessary to control for weight. It surrounds the urethra just below the urinary bladder and can be felt during a rectal exam.
Divisions (?????)
One can sub-divide the prostate in two ways: by zone or by lobe. It does not have a capsule; rather an integral fibromuscular band surrounds it, which is sheathed in the muscles of the pelvic floor, which contract during the ejaculatory process.
Zones (???????)
The “zone” classification is more often used in pathology. John E. McNeal first proposed the idea of “zones” in 1968. McNeal found that the relatively homogeneous cut surface of an adult prostate in no way resembled “lobes” and thus led to the description of “zones”.
The prostate gland has four distinct glandular regions, two of which arise from different segments of the prostatic urethra:
| Name | Fraction of gland | Description |
| Peripheral zone (PZ) | Up to 70% in young men | The sub-capsular portion of the posterior aspect of the gland that surrounds the distal urethra. From this portion of the gland ~70–80% of prostatic cancers originate. |
| The central zone (CZ) | Approximately 25% normally | This zone surrounds the ejaculatory ducts. The central zone accounts for roughly 2.5% of cancers; these cancers tend to be more aggressive and more likely to invade the seminal vesicles. |
| Transition zone (TZ) | 5% at puberty | ~10–20% of prostate cancers originate in this zone. The transition zone surrounds the proximal urethra and is the region of the prostate gland that grows throughout life and causes the disease of benign prostatic enlargement. |
| Anterior fibro-muscular zone (or stroma) | Approximately 5% | This zone is usually devoid of glandular components, and composed only, as its name suggests, of muscle and fibrous tissue. |
Lobes (???????)
The “lobe” classification is more often used in anatomy. The prostate is incompletely divided into five lobes:
| Anterior Lobe | Roughly corresponds to part of the transitional zone |
| Posterior Lobe | Roughly corresponds to the peripheral zone |
| Right & left Lateral lobes | Span all zones |
| Median Lobe | Roughly corresponds to part of the central zone |
Prostate Development (????? ?????? ?? ?????)
The prostatic part of the urethra develops from the middle part of the urogenital sinus. Endodermal outgrowths arise from the prostatic part of the urethra and grow into the surrounding mesenchyme. The glandular epithelium of the prostate differentiates from these endodermal cells, and the associated mesenchyme differentiates into the dense stroma and the smooth muscle.
The glands represent the modified wall of the proximal portion of the male urethra and arise by the 9th week of embryonic life in the development of the reproductive system. Condensation of mesenchyme, urethra and Wolffian ducts gives rise to the adult gland, a composite organ made up of several glandular and non-glandular components tightly fused.
Prostate Function (????? ?????? ?? ?????)
Male sexual response (????? ?? ??? ???????????)
During male seminal emission, sperm is transmitted from the vas deferens into the male urethra via the ejaculatory ducts, which lie within the prostate gland. Ejaculation is the expulsion of semen from the urethra. It is possible for some men to achieve orgasm solely through stimulation of the prostate gland, such as massage or anal intercourse.
Secretions (?????)
Prostatic secretions vary among species. They are generally composed of simple sugars and are often slightly alkaline. In human prostatic secretions, the protein content is less than 1% and includes:
- Proteolytic enzymes
- Prostatic acid phosphatase
- Beta-microseminoprotein
- Prostate-specific antigen
The secretions also contain zinc with a concentration of 500–1,000 times the concentration in blood.
Regulation (???????)
To function properly, the prostate needs male hormones, which are responsible for male sex characteristics. The main male hormone is testosterone, which is produced mainly by the testicles. It is dihydrotestosterone (DHT), a metabolite of testosterone, that predominantly regulates the prostate.
Gene and protein expression (??? ?? ??????? ??????????)
About 20,000 protein-coding genes are expressed in human cells and almost 75% of these genes are expressed in the normal prostate. About 150 of these genes are more specifically expressed in it with about 20 genes being highly prostate-specific.
The corresponding specific proteins are expressed in the glandular and secretory cells of the prostatic gland and have functions that are important for the characteristics of semen. Examples of some of the most prostate-specific proteins are enzymes, such as the prostate-specific antigen (PSA), and the ACPP protein.
Clinical significance (??????? ?????)
A volume of over 30 cm3 is regarded as prostatomegaly (enlarged prostate). Prostatomegaly can be due to any of the following conditions.
Enlargement (??????)
Prostatitis is enlargement of the gland. There are primarily four different forms of prostatitis, each with different causes and outcomes. Two relatively uncommon forms, acute prostatitis, and chronic bacterial prostatitis are treated with antibiotics (category I and II, respectively).
Chronic non-bacterial prostatitis or male chronic pelvic pain syndrome (category III), which comprises about 95% of prostatitis diagnosis, is treated by a large variety of modalities including:
- Alpha-blockers
- Physical therapy
- Psychotherapy
- Antihistamines
- Anxiolytics
- Nerve modulators
- Phytotherapy
- Surgery, and more
More recently, a combination of trigger point and psychological therapy has proved effective for category III prostatitis as well. Category IV prostatitis, relatively uncommon in the general population, is a type of leukocytosis.
Benign prostatic hyperplasia (????? ?????? ??? ?????????)
Benign prostatic hyperplasia (BPH) occurs in older men; the prostate often enlarges to the point where urination becomes difficult. If the prostate grows too large, it may constrict the urethra and impede the flow of urine, making urination difficult and painful and, in extreme cases, completely impossible.
Lifestyle changes to improve the quality of urination include urinating in the sitting position. This reduces the amount of residual volume in the bladder, increases the urinary flow rate and decreases the voiding time.
Prostate Cancer (????? ?????? ?? ?????)
Prostate cancer is one of the most common cancers affecting older men in developed countries and a significant cause of death for elderly men. Screening for cancer may be in the form of a physical rectal examination or measurement of PSA level in the blood, however, given the significant risk of overdiagnosis with widespread screening in the general population, prostate cancer screening is controversial.
Prostate Massage (????? ?????? ?? ?????)
Massage or stimulation of the male prostate gland for medical purposes or sexual stimulation. The prostate takes part in the sexual response cycle and is essential for the production of semen. Due to its proximity to the anterior rectal wall, it can be stimulated from the anterior wall of the rectum or externally via the perineum.

- Reference: https://en.wikipedia.org/wiki/Prostate

It’s new thing for me to know about a role of prostate. Very nicely explained. Thank you very much for this precious knowledge.
Nicely explained
Покупка диплома о среднем полном образовании: как избежать мошенничества?
wayworld.listbb.ru/viewtopic.php?f=2&t=27102
Приобретение школьного аттестата с официальным упрощенным обучением в Москве