Inflammation (सूजन और जलन) is part of the complex biological response of body tissues to harmful stimuli, such as pathogens, damaged cells, or irritants, and is a protective response involving immune cells, blood vessels, and molecular mediators. The function of inflammation is to eliminate the initial cause of cell injury, clear out necrotic cells and tissues damaged from the original insult and the inflammatory process, and initiate tissue repair. Inflammation has also been classified as Type 1 and Type 2 based on the type of cytokines and helper T cells (Th1 and Th2) involved. The inflammation–infection distinction becomes crucial for situations in pathology and medical diagnosis where inflammation is not driven by microbial invasions, such as the cases of atherosclerosis, trauma, ischemia, and autoimmune diseases (including type III hypersensitivity).
Inflammation Meaning
Inflammation refers to the body’s natural response to injury, infection, or irritation. It is a vital part of the immune system and plays a crucial role in protecting the body from harmful stimuli and promoting healing. The term “inflammation” comes from the Latin word “inflammare,” which means to set on fire.
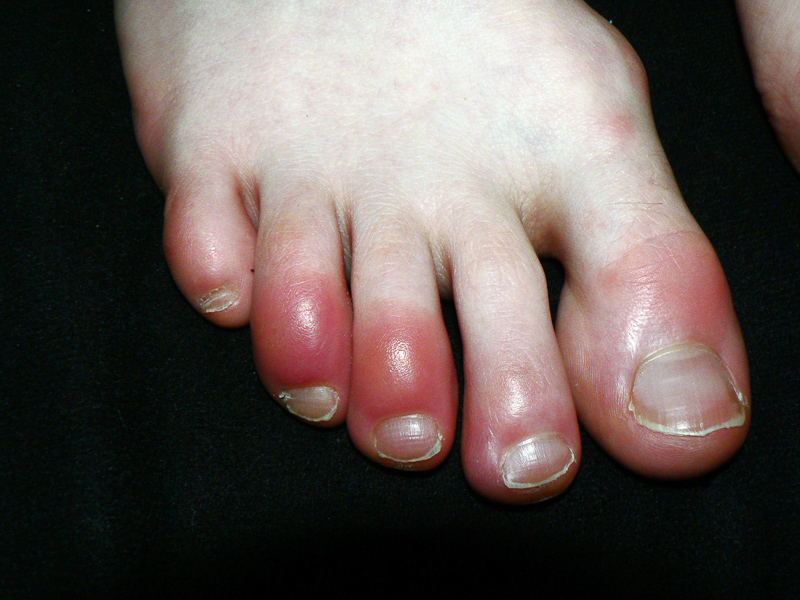
Inflammation Types
Inflammation can be classified into several types based on different criteria. Here are some common types of inflammation:
Acute Inflammation
This is the most common type and occurs as a short-term response to injuries or infections. It typically starts rapidly and lasts for a few days or weeks. The signs of acute inflammation include redness, swelling, heat, pain, and loss of function at the affected site. Examples of conditions that cause acute inflammation include a sprained ankle, a sore throat due to a viral infection, or a cut on the skin.
Chronic Inflammation
Unlike acute inflammation, chronic persists over a more extended period, often for months or even years. It can result from unresolved acute inflammation, ongoing exposure to irritants or toxins, or autoimmune disorders where the immune system attacks the body’s tissues. Chronic can lead to tissue damage and is associated with various diseases such as rheumatoid arthritis, inflammatory bowel disease (IBD), and chronic obstructive pulmonary disease (COPD).
Systemic Inflammation
This type affects the whole body and not just a specific area. It is often associated with infections or diseases that release inflammatory markers into the bloodstream. Systemic inflammation can cause symptoms such as fever, fatigue, loss of appetite, and muscle aches. Conditions like sepsis, a severe response to infection, can lead to systemic inflammation.
Sterile Inflammation
In some cases, it can occur without the presence of infectious agents. Sterile inflammation may result from non-infectious injuries or conditions, such as burns, autoimmune diseases, or exposure to certain chemicals.
Granulomatous Inflammation
This type is characterized by the formation of granulomas, which are small nodules composed of immune cells. Granulomas are the body’s attempt to contain and isolate certain substances that cannot be eradicated. Examples of diseases associated with granulomatous inflammation include tuberculosis and sarcoidosis.
Allergic Inflammation
Allergies trigger a specific type of response when the immune system overreacts to harmless substances like pollen, pet dander, or certain foods. Allergic inflammation can lead to symptoms such as itching, sneezing, wheezing, and skin rashes.
Each type has distinct characteristics and underlying causes, and understanding these differences is crucial for accurate diagnosis and appropriate treatment. If you suspect it or any related health concerns, it’s essential to seek medical advice from a healthcare professional.
Inflammation Symptoms
The symptoms can vary depending on the type and location. However, some common symptoms associated with this include:
Redness (Rubor)
The affected area may appear red due to increased blood flow to the site. This happens because blood vessels in the area dilate to allow more immune cells to reach the site of injury or infection.
Swelling (Tumor)
Inflammation often leads to the accumulation of fluid and immune cells at the site, causing swelling or edema. Swelling is the body’s way of isolating the injured or infected area and protecting it from further damage.
Heat (Calor)
Increased blood flow to the affected area can cause it to feel warm to the touch. This localized heat is a result of the body’s immune response.
Pain (Dolor)
Inflammation can trigger the release of chemicals that activate nerve endings, leading to pain or discomfort in the affected area. Pain serves as a warning sign, discouraging the use of the injured area and promoting rest for healing.
Loss of Function (Functio Laesa)
In some cases, inflammation can impair the normal function of the affected area. For example, a swollen joint might limit its range of motion or a sore throat may make swallowing difficult.
Fever
Systemic inflammation, such as during infections, can lead to an increase in body temperature, resulting in a fever. Fever is part of the body’s defense mechanism to combat infections by creating an environment less favorable for invading pathogens.
Fatigue
Chronic, especially systemic inflammation, can cause feelings of tiredness and fatigue as the body expends energy to combat the ongoing inflammatory response.
Other Symptoms
Depending on the cause and location of inflammation, other symptoms may be present. For instance, inflammation in the respiratory tract can lead to coughing and difficulty breathing, while inflammation in the gastrointestinal tract can cause abdominal pain and changes in bowel movements.
It’s important to note that these symptoms are part of the body’s natural defense mechanism to protect and heal itself. However, if it becomes chronic or leads to severe discomfort or complications, it’s essential to seek medical attention for proper diagnosis and treatment. Additionally, symptoms can sometimes be similar to those of other conditions, so a healthcare professional’s evaluation is necessary for an accurate diagnosis.

Inflammation Causes
It can be caused by a wide range of factors, including:
Infections
Bacterial, viral, fungal, or parasitic infections can trigger an immune response and lead to inflammation. The body releases various immune cells and chemicals to combat the invading pathogens and clear the infection.
Injuries
Physical injuries, such as cuts, burns, bruises, or fractures, can cause it as the body initiates the healing process. Inflammation helps to remove damaged tissue and initiate tissue repair.
Tissue Damage
Any form of tissue damage, whether due to trauma, surgery, or certain medical conditions, can lead to inflammation. The body responds to the damaged cells by activating the immune system.
Autoimmune Diseases
In autoimmune disorders, the immune system mistakenly attacks the body’s healthy tissues, leading to chronic inflammation. Examples of autoimmune diseases include rheumatoid arthritis, lupus, and multiple sclerosis.
Allergic Reactions
When the immune system overreacts to harmless substances like pollen, dust, pet dander, or certain foods, it can trigger allergic reactions. Allergies often involve inflammation as part of the body’s response to the perceived threat.
Chronic Irritants
Prolonged exposure to irritants such as tobacco smoke, air pollution, chemicals, or certain allergens can cause chronic inflammation in affected tissues.
Obesity
Excess body fat resulting in obesity, especially visceral fat around organs, can release inflammatory chemicals, leading to low-grade chronic inflammation throughout the body.
Stress
Chronic stress can contribute to inflammation as it activates the release of stress hormones, which can influence the immune system‘s response.
Inflammatory Diseases
Some conditions are characterized by chronic inflammation, such as inflammatory bowel disease (IBD), psoriasis, and asthma.
Toxins
Exposure to certain toxins and pollutants can trigger an inflammatory response in the body.
Chronic Infections
In some cases, the body may struggle to eliminate certain infections completely, leading to chronic low-grade inflammation as the immune system tries to control the persistent pathogens.
It’s important to recognize that it is a normal and necessary process for the body to protect itself and promote healing. However, when it becomes chronic or excessive, it can lead to various health problems and contribute to the development of certain diseases. Managing underlying causes and adopting a healthy lifestyle can play a significant role in reducing the risk and related health issues. If you are experiencing chronic inflammation or have concerns about your health, consult a healthcare professional for evaluation and appropriate management.
Inflammation Diagnosis
The diagnosis involves a comprehensive assessment of the patient’s medical history, physical examination, and sometimes additional tests. The goal is to determine the presence, location, and possible cause. Here’s an overview of the steps involved in the diagnosis:
Medical History
The healthcare professional will begin by taking a detailed medical history, including any current symptoms, past medical conditions, family history of inflammatory diseases, recent infections or injuries, and medication use.
Physical Examination
A thorough physical examination will be performed to assess the affected area(s) and look for signs, such as redness, swelling, warmth, pain, and loss of function. The doctor may also check for signs of systemic inflammation, such as fever or enlarged lymph nodes.
Laboratory Tests
Blood tests can be helpful in assessing inflammation. Commonly used blood markers include C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR). These markers tend to be elevated in response.
Imaging Studies
Depending on the suspected location and cause, imaging tests like X-rays, ultrasound, CT scans, or MRI may be ordered to visualize the affected area and detect any structural changes or abnormalities.
Biopsy
In some cases, a tissue biopsy may be necessary to confirm the presence of inflammation and to identify the underlying cause. During a biopsy, a small sample of the affected tissue is taken and examined under a microscope.
Allergy Testing
If it is suspected to be due to an allergic reaction, allergy testing may be performed to identify specific allergens responsible for triggering the immune response.
Autoantibody Testing
In cases where autoimmune diseases are suspected, testing for specific autoantibodies can help in the diagnosis of the particular condition.
Culture and Microbial Testing
If an infection is suspected as the cause of inflammation, cultures of blood, urine, or other body fluids may be collected to identify the specific pathogen responsible.
Elimination Diet or Food Allergy Testing
In cases of suspected food-related inflammation or allergies, an elimination diet or food allergy testing may be recommended.
Functional Testing
In functional medicine, specialized tests may be used to assess various aspects of inflammation, oxidative stress, and immune function.
It’s important to note that it can be a symptom of various underlying conditions, so an accurate diagnosis is essential for proper management and treatment. If you experience symptoms or have concerns about your health, it is advisable to seek medical attention and consult with a healthcare professional for a thorough evaluation and diagnosis.
Inflammation Prevention
Prevention involves adopting a healthy lifestyle and making choices that promote overall well-being. While it may not be possible to prevent all types, the following practices can help reduce the risk of chronic inflammation and its associated health issues:
Maintain a Balanced Diet
Focus on a diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats. Antioxidant-rich foods, such as berries, leafy greens, and nuts, can help reduce oxidative stress, which can contribute to inflammation. Minimize the intake of processed foods, sugary beverages, and trans fats, as they can promote it.
Regular Exercise
Engage in regular physical activity to help maintain a healthy weight and reduce inflammation. Exercise can also enhance the immune system and promote overall well-being.
Manage Stress
Chronic stress can contribute to inflammation. Incorporate stress-reducing practices into your daily routine, such as mindfulness meditation, deep breathing exercises, yoga, or spending time in nature.
Get Adequate Sleep
Aim for 7-9 hours of quality sleep each night. Proper rest is essential for immune function and overall health.
Avoid Tobacco and Limit Alcohol
Smoking and excessive alcohol consumption can increase inflammation and have detrimental effects on health. Quit smoking and limit alcohol intake to moderate levels.
Maintain a Healthy Weight
Obesity is associated with increased inflammation. By maintaining a healthy weight through diet and exercise, you can reduce the risk.
Regular Check-ups
Schedule regular check-ups with your healthcare provider to monitor your overall health and address any potential health issues promptly.
Limit Exposure to Toxins
Minimize exposure to environmental toxins and pollutants whenever possible. Use natural cleaning products and avoid exposure to secondhand smoke.
Practice Good Hygiene
Follow proper hygiene practices to reduce the risk of infections that can lead to inflammation.
Treat Infections Promptly
If you have an infection, seek appropriate medical treatment to prevent it from becoming severe or chronic.
Manage Chronic Conditions
If you have a chronic condition, work closely with your healthcare provider to manage it effectively and prevent complications that could lead to inflammation.
Anti-inflammatory Supplements
Some supplements, such as omega-3 fatty acids, curcumin, and ginger, have anti-inflammatory properties. Consult with a healthcare professional before starting any supplements.
Remember that individual factors, genetics, and underlying health conditions can influence inflammation. While these preventive measures can help reduce the risk of chronic inflammation, it’s essential to work with a healthcare provider to tailor a plan that suits your specific needs and health status. If you have concerns about it or related health issues, consult a healthcare professional for personalized advice and recommendations.
Inflammation Management
Managing it involves a combination of lifestyle changes, medical treatments, and self-care strategies. The specific approach to management will depend on the underlying cause and the severity. Here are some general strategies for managing inflammation:
Medications
Depending on the type and cause, over-the-counter or prescription medications may be used to reduce inflammation and manage symptoms. Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help with mild inflammation, while corticosteroids may be prescribed for more severe cases.
Physical Therapy
For musculoskeletal inflammation or injuries, physical therapy can be beneficial. It involves exercises and techniques to improve flexibility, strength, and mobility, helping to reduce it and promote healing.
Rest
Giving the affected area or the body, in general, sufficient rest is crucial for allowing the inflammation to subside and promoting healing.
Cold and Heat Therapy
Applying ice packs to the affected area can help reduce swelling and numb pain. On the other hand, heat therapy with warm compresses or heating pads can promote blood circulation and ease muscle tension.
Anti-inflammatory Diet
Adopting an anti-inflammatory diet can be helpful for managing chronic inflammation. Focus on foods rich in antioxidants, such as fruits, vegetables, nuts, and seeds, and reduce the intake of processed foods, sugar, and trans fats.
Regular Exercise
Engage in regular physical activity, as it can help reduce inflammation and support overall health. Low-impact exercises like walking, swimming, or yoga can be particularly beneficial for individuals.
Stress Management
Chronic stress can exacerbate inflammation. Practice stress-reduction techniques such as meditation, deep breathing, or engaging in hobbies to promote relaxation.
Weight Management
If overweight, losing excess weight can reduce inflammation, particularly in cases of obesity-related inflammation.
Smoking Cessation
Quitting smoking can significantly reduce inflammation and improve overall health.
Avoid Triggers
If certain substances or allergens trigger inflammation or allergic reactions, avoid exposure to them whenever possible.
Medical Treatment for Underlying Conditions
For inflammation related to autoimmune diseases or chronic conditions, following prescribed treatment plans and medications is essential for managing inflammation effectively.
Anti-inflammatory Supplements
Some individuals may benefit from supplements with anti-inflammatory properties, such as omega-3 fatty acids, turmeric, or ginger. However, always consult with a healthcare professional before starting any supplements.
Regular Check-ups
Schedule regular check-ups with your healthcare provider to monitor inflammation and overall health. It allows for early detection of any changes that may require adjustments to the management plan.
Remember that the management should be tailored to the individual’s specific needs and health condition. If you have chronic inflammation or concerns about your health, consult with a healthcare professional for a comprehensive evaluation and personalized management plan.
Inflammation Treatment
The treatment depends on the underlying cause, the severity, and the affected area. In some cases, it may resolve on its own with self-care measures, while in other instances, medical intervention is necessary. Here are some common treatment approaches:
Rest and Self-care
For mild cases, rest and self-care may be sufficient. This includes avoiding activities that exacerbate the inflammation, applying ice packs or warm compresses, and using over-the-counter pain relievers (e.g. acetaminophen, ibuprofen) as directed.
Medications
Anti-inflammatory medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen, can help reduce inflammation and alleviate pain. For more severe cases or those related to autoimmune diseases, corticosteroids or disease-modifying antirheumatic drugs (DMARDs) may be prescribed.
Physical Therapy
Physical therapy can be beneficial for musculoskeletal injuries. A physical therapist can develop a personalized exercise and stretching program to promote healing and improve strength and flexibility.
Immunosuppressants
In cases of chronic inflammation associated with autoimmune disorders, immunosuppressive medications may be used to help control the immune response and reduce inflammation.
Biologic Therapies
Biologic drugs are a type of targeted therapy that can be used to treat certain autoimmune conditions by blocking specific inflammatory pathways.
Antibiotics
If inflammation is caused by a bacterial infection, antibiotics may be prescribed to eliminate the infection and reduce it.
Allergy Medications
Antihistamines and other allergy medications can help manage inflammation related to allergic reactions.
Lifestyle Changes
Adopting a healthy lifestyle, including a balanced diet, regular exercise, stress management, and sufficient sleep, can help reduce inflammation and improve overall health.
Weight Management
For individuals with obesity-related inflammation, weight loss through a combination of diet and exercise can be beneficial.
Surgery
In some cases, surgical intervention may be necessary to address the underlying cause, such as removing infected tissue or repairing damaged structures.
Complementary and Alternative Therapies
Some people find relief from inflammation through complementary therapies like siddha remedies, acupuncture, chiropractic care, or herbal remedies. However, it’s essential to consult with a healthcare professional before trying these approaches.
The appropriate treatment varies depending on the individual’s specific condition and health status. If you experience persistent or severe inflammation or have concerns about your health, it’s crucial to seek medical advice from a qualified healthcare professional for a proper diagnosis and treatment plan. Self-medication and unproven treatments can be harmful and may not effectively address the underlying cause.
Ayurveda Treatment for Inflammation
Reference: https://en.wikipedia.org/wiki/Inflammation

Покупка школьного аттестата с упрощенной программой: что важно знать
asg-amt.phorum.pl/viewtopic.php?p=33503#33503
Вопросы и ответы: можно ли быстро купить диплом старого образца?
vsetutonline.com/forum/member.php?u=76509