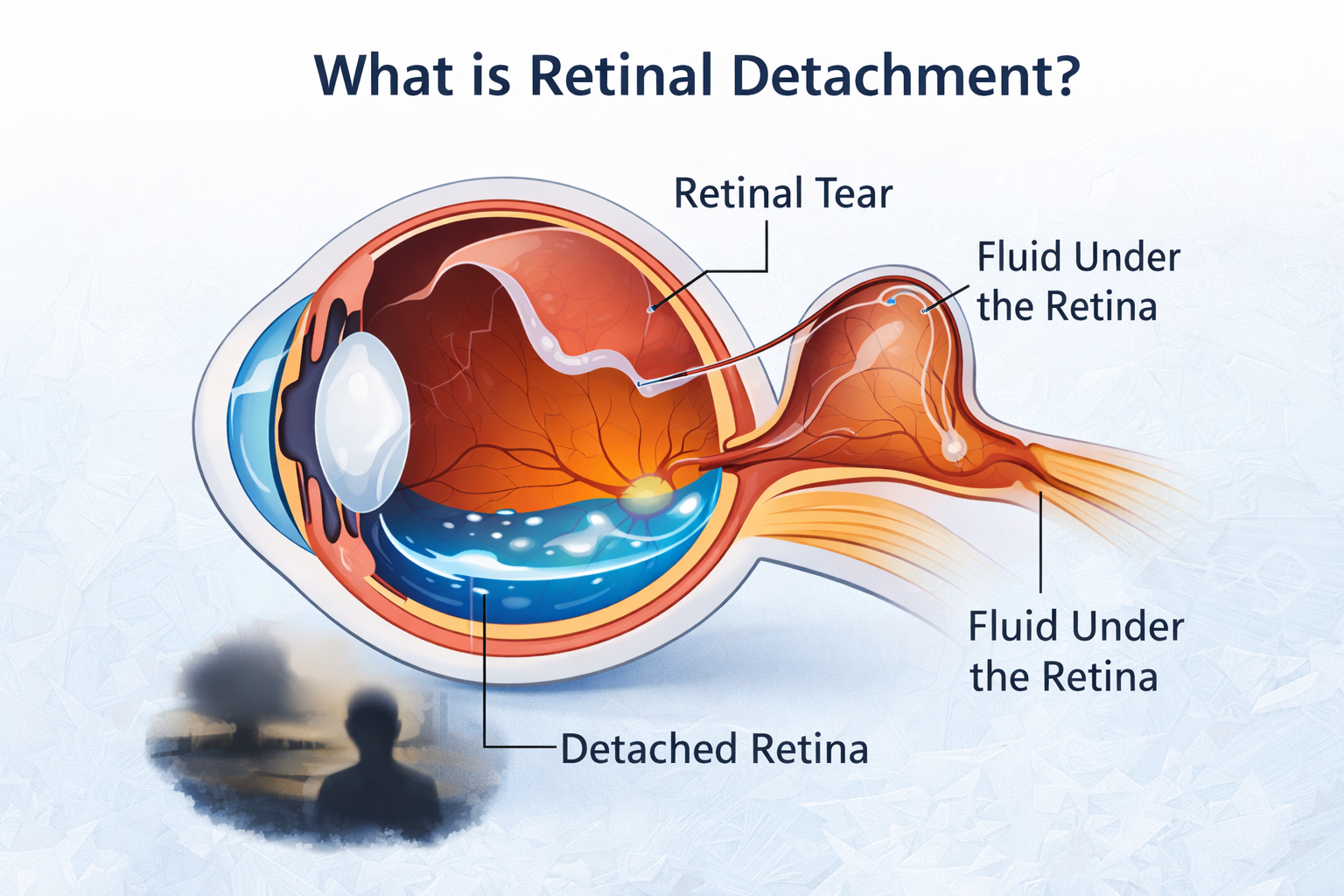
Retinal detachment (रेटिना का अलग होना) is a condition in which the retina pulls away from the tissue beneath it. It may start in a small area, but without quick treatment, it can spread across the entire retina, leading to serious vision loss and possibly blindness. Retinal detachment is a medical emergency that requires surgery. The retina is a thin layer at the back of the eye that processes visual information and sends it to the brain. When the retina detaches, common symptoms include seeing floaters, flashes of light, a dark shadow in vision, and sudden blurred vision. The most common type of retinal detachment is rhegmatogenous, which occurs when a tear or hole in the retina allows fluid from the center of the eye to enter the subretinal space, causing the retina to detach.
Rhegmatogenous retinal detachment is most commonly caused by posterior vitreous detachment, a condition where the gel inside the eye breaks down and pulls on the retina. Risk factors include older age, nearsightedness (myopia), eye injury, cataract surgery, and inflammation.
What Is Retinal Detachment?
Retinal detachment is a medical emergency in which the retina separates from the underlying layer of tissue that provides it with oxygen and nutrients. The retina is the light-sensitive tissue located at the back of the eye. It captures light signals and sends them to the brain via the optic nerve, enabling vision.
When the retina detaches, it can no longer function properly. If left untreated, the detached portion of the retina may suffer permanent damage, leading to partial or complete vision loss.
Understanding the Retina and Its Function
The retina works like the film in a camera (or the sensor in a digital camera). It converts light into electrical signals that are interpreted by the brain.
Key components include:
-
Photoreceptor cells (rods and cones)
-
Macula – responsible for central, detailed vision
-
Peripheral retina – responsible for side vision
-
Optic nerve – transmits visual signals to the brain
When the retina separates from the underlying retinal pigment epithelium (RPE), it loses its blood supply. Without immediate medical attention, the affected cells can die.
Types of Retinal Detachment
There are three main types of retinal detachment:
Rhegmatogenous Retinal Detachment
This is the most common type. It occurs due to a tear or break in the retina. Fluid passes through the tear and accumulates underneath the retina, causing it to separate.
It is often associated with:
-
Aging
-
Severe nearsightedness (high myopia)
-
Trauma
-
Posterior vitreous detachment (PVD)
Tractional Retinal Detachment
This occurs when scar tissue on the retina’s surface contracts and pulls the retina away from the back of the eye.
Common causes include:
-
Eye infections
-
Previous eye surgeries
Exudative (Serous) Retinal Detachment
In this type, fluid accumulates beneath the retina without any tear or break. It is often caused by:
-
Inflammatory disorders
-
Tumors
-
Severe hypertension
-
Age-related macular degeneration
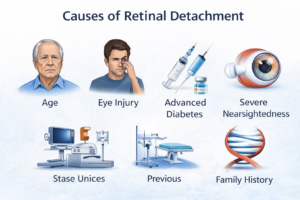
Causes of Retinal Detachment
Retinal detachment can occur due to several factors:
-
Age-related changes in the vitreous gel
-
Eye injury or trauma
-
Advanced diabetes
-
Severe myopia (nearsightedness)
-
Previous eye surgery (such as cataract surgery)
-
Family history of retinal detachment
-
Inflammatory eye diseases
As people age, the vitreous gel inside the eye shrinks and may pull away from the retina. In some cases, this pulling creates a tear that leads to detachment.
Risk Factors
Certain individuals are more prone to retinal detachment:
-
Age above 50
-
High myopia
-
History of retinal detachment in one eye
-
Family history
-
Eye trauma
-
Diabetic retinopathy
-
Causes, risk of prior eye surgery
If you fall into any of these categories, regular eye checkups are essential.
Symptoms of Retinal Detachment
Retinal detachment usually develops suddenly and painlessly. Warning signs include:
Sudden Increase in Floaters
You may notice small dark spots, cobweb-like shapes, or specks floating in your field of vision.
Flashes of Light (Photopsia)
Brief flashes of light in peripheral vision may indicate retinal pulling.
A Shadow or Curtain Over Visioncauses, riskfactors,
Many patients describe it as a gray curtain moving across their vision.
Blurred or Distorted Vision
Central vision may become distorted if the macula is affected.
Sudden Loss of Peripheral Vision
Side vision may gradually decrease.
If you experience any of these symptoms, seek immediate medical care.
How Is Retinal Detachment Diagnosed?
An ophthalmologist performs a comprehensive eye examination that may include:
-
Dilated eye examination
-
Indirect ophthalmoscopy
-
Ultrasound imaging (if bleeding blocks view)
-
Optical coherence tomography (OCT)
Early detection significantly improves treatment outcomes.
Treatment Options for Retinal Detachment
Retinal detachment requires prompt medical or surgical treatment. The choice depends on severity and type.
Laser Photocoagulation
Used for small retinal tears. A laser seals the tear to prevent fluid from entering.
Cryopexy
A freezing treatment that creates a scar to seal retinal breaks.
Pneumatic Retinopexy
A gas bubble is injected into the eye to push the retina back into place. The patient must maintain a specific head position for several days.
Scleral Buckling
A silicone band is placed around the eye to counteract the force pulling the retina away.
Vitrectomy
The vitreous gel is removed and replaced with gas or silicone oil. This procedure is common in complex cases.
Modern surgical techniques have a high success rate, especially when treated early.
Recovery After Retinal Detachment Surgery
Recovery depends on the type of surgery performed.
Common recovery considerations:
-
Avoid heavy lifting
-
Maintain prescribed head positioning (if a gas bubble is used)
-
Use prescribed eye drops
-
Avoid air travel (if a gas bubble is present)
-
Attend follow-up appointments
Vision may take weeks or months to improve.
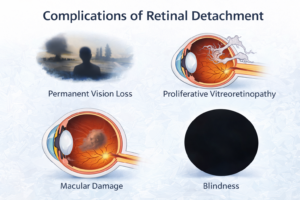
Complications of Untreated Retinal Detachment
If left untreated, retinal detachment can cause:
-
Permanent vision loss
-
Proliferative vitreoretinopathy (scar tissue formation)
-
Macular damage
-
Blindness
Prompt intervention is crucial to preserving eyesight.
Can Retinal Detachment Be Prevented?
While not all cases are preventable, you can reduce risk by:
-
Regular eye examinations
-
Managing diabetes
-
Wearing protective eyewear during sports
-
Treating retinal tears early
-
Controlling high blood pressure
If you are at high risk, your ophthalmologist may recommend periodic retinal evaluations.
Retinal Detachment and Diabetes
People with diabetes are at higher risk due to diabetic retinopathy. Scar tissue formation can pull on the retina, leading to tractional detachment.
Proper blood sugar control and annual retinal screening significantly reduce risk.
Retinal Detachment vs Posterior Vitreous Detachment (PVD)
Posterior vitreous detachment (PVD) is common with aging and does not always lead to retinal detachment. However, in some cases, it can cause retinal tears.
Symptoms of both conditions may appear similar, so professional evaluation is necessary.
Prognosis and Long-Term Outlook
The visual outcome depends on:
-
How quickly treatment is initiated
-
Whether the macula was involved
-
Overall eye health
If treated before the macula detaches, vision recovery is often excellent. Delayed treatment reduces the chance of full recovery.
Conclusion
Retinal detachment is a serious but treatable eye condition. Early recognition of symptoms such as flashes, floaters, and shadowed vision can make the difference between full recovery and permanent vision loss.
With modern surgical advancements, the prognosis for detachment has improved significantly. However, timely diagnosis remains the key factor in preserving eyesight.
Regular eye checkups, especially for high-risk individuals, are essential. If you experience sudden vision changes, do not ignore them—consult an ophthalmologist immediately.
Protecting your vision starts with awareness. Understanding detachment empowers you to act quickly and safeguard your eyesight for the future.
Frequently Asked Questions (FAQs)
1. Is retinal detachment painful?
No, it is usually painless because the retina lacks pain-sensitive nerves. However, it often causes sudden visual symptoms like flashes of light, floaters, or a shadow across vision. These warning signs should never be ignored.
2. How urgent is retinal detachment?
It is a medical emergency that requires immediate attention. Delaying treatment can lead to permanent vision loss, especially if the macula becomes detached. Early surgical intervention significantly improves visual outcomes.
3. Can retinal detachment heal on its own?
No, it cannot heal naturally without medical or surgical treatment. Once the retina separates from its blood supply, it needs prompt repair to prevent permanent damage. Waiting for it to improve on its own can worsen vision loss.
4. How long does retinal detachment surgery take?
Most detachment surgeries take about 1 to 2 hours, depending on the type and severity of the detachment. Procedures such as vitrectomy or scleral buckle may vary slightly in duration. Many are performed under local or general anesthesia.
5. Can retinal detachment be prevented?
While not always preventable, regular eye exams can help detect retinal tears before detachment occurs. Managing diabetes, protecting the eyes from injury, and monitoring sudden vision changes reduce the risk. Early treatment of retinal breaks is key.
6. Is retinal detachment common?
It is relatively uncommon but becomes more likely with age, especially after 50. It is more frequent in people with high myopia, previous eye surgery, or trauma. Though rare, it remains a serious vision-threatening condition.
7. Can retinal detachment occur in both eyes?
Yes, it can occur in both eyes, particularly in individuals with strong risk factors such as severe myopia or a family history. If one eye is affected, the other eye may also be at higher risk. Regular monitoring is important.
8. What is the success rate of retinal detachment surgery?
Modern retinal surgeries have a high success rate, often above 85–90% with a single procedure. Some complex cases may require additional surgery. Early detection and treatment greatly improve the final visual result.
9. Can vision return to normal after retinal detachment?
Vision recovery depends on how quickly treatment is provided and whether the macula was involved. If treated early before central vision is affected, recovery can be very good. Delayed treatment may result in permanent visual impairment.
10. Is retinal detachment hereditary?
A family history can increase your risk, especially if associated with inherited eye conditions or high myopia. However, not all cases are genetic. Regular screening is advisable if there is a known family history.
Reference: https://en.wikipedia.org/wiki/Retinal_detachment